Lumbar stenosis
What causes Lumbar stenosis (spinal canal narrowing)?
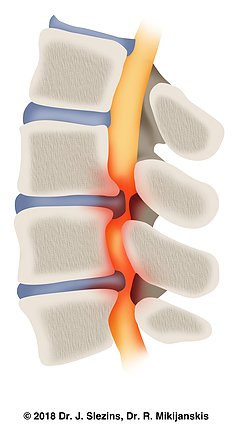
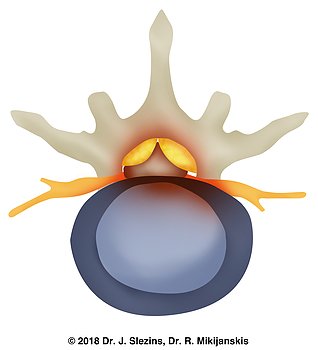
The lumbar spine consists of 5 or less commonly 6 vertebrae located between the thorax and the pelvis. The spinal cord, which is located within a canal inside the spine (spinal canal) ends at the level of the 12th thoracic vertebra in men and at the 1st lumbar vertebra in women. Below this level, the spinal cord continues with multiple lumbar and sacral nerves (all together also called a cauda equina) also located within the spinal canal. The narrowing of the spinal canal and impingement of the nerves located within this canal is called Spinal Lumbar Stenosis. Most commonly lower segments of the lumbar spine are affected since they take the brunt of the downward force excreted on the spine. The nerves located in this segment are responsible for the innervation of the legs, which explains the typical presentation of symptoms below the level of compression.
The narrowing of the spinal canal in the elderly is mostly a gradual process. Each element of the vertebrae and their joints have a particular role to play in providing support, motion, cushioning, and protection of nerve structures. Individual aging processes, hard physical labor, and/or sedentary lifestyles lead to gradual inflammatory and degenerative changes in these structures. This, in turn, leads to a gradual decrease in the height of the intervertebral discs, their ductal canalization, enlargement of the intervertebral joints, the formation of osteophytes or ‘bone spurs’, and the thickening of the spinal ligaments. The culmination of all these changes is spinal stenosis.
The narrowing of the spinal canal and lumbar spine stenosis is one of the most common problems affecting the quality of life in the elderly.
At what age does the disease occur?
The typical age of manifestation is 60 (the/after the 6th decade of life), but due to various congenital and lifetime problems of the spine, this disease can also manifest itself in younger patients.
What are the symptoms of Lumbar stenosis?
The disease is characterized by a decrease in walking distance – a gradually decreasing distance that can be walked without stopping, resting, or sitting down. This decrease in walking distance is most commonly associated with leg and low back pain, however, it may be completely painless (extreme feeling of tiredness in the legs), but may also be manifested by transient weakness, pain, and numbness in the legs (patients sometimes call it ‘inflammation of the sciatic nerve’), severe pain in the lumbar spine. Complaints and symptoms, including sciatica if present are remitted by rest.
A common sign of this disease is cramping in the muscles of the lower leg. Cramps can be caused by walking or exercising, but they also occur at rest, such as when sleeping at night.
In rare cases, the disease can cause permanent problems with the movement of the legs, the bowel, and the bladder problems, such as incontinence (cauda equina syndrome).
Back pain is often not a direct sign of spinal stenosis, but can often be associated with degenerative (aging) processes of the spine, such as inflammation of the intervertebral facet joints.
How is spinal canal stenosis diagnosed?
The doctor first suspects this diagnosis after a thorough questioning and examination of the patient. The signs of lumbar stenosis are very similar and, without further examination, are often indistinguishable from narrowing or occlusion of the leg arteries. The general practitioner may order an x-ray and/or CT scan of the lumbar spine before referral to a specialist. These examinations often have no confirmatory role in diagnosis, but they may indicate the direction in which further diagnosis should be made. Magnetic resonance imaging (MRI) is the gold standard for radiological examination, without which a complete diagnosis and consequent evaluation of appropriate treatment of this disease is unimaginable today. Patients are usually referred to magnetic resonance imaging by a specialist doctor.
What are the treatment options for this disease?
Studies have shown that vertebral canal narrowing does not always warrant immediate surgery. A specialist will be there to help you to decide which type of treatment will be best for you.
If the problem does not cause, for example, a significant decrease in quality of life (very short walking distance, severe pain, weakness in the legs) and loss of working capacity, your doctor may give you advice for initial types of therapy, before surgery is attempted. This treatment includes medication and physical therapy. The patient may also be advised to make appropriate lifestyle changes – such as smoking cessation and weight loss.
In case there is a need for our specialist opinion, we are happy to help. We provide appointments and consultations for both – residents of Latvia and patients from abroad, including remote appointments via video call. There are a number of ways to schedule an appointment with one of our specialists, electronically (for Latvian residents) or by requesting a remote appointment via video call email, or telephone contact.
When is an operation required for Lumbar stenosis?
Surgery is required when the patient has symptoms that interfere with normal daily activities, significantly restricting the ability to move and/or decrease the walking distance. Surgery is considered if all previous treatment methods/options have failed to yield adequate results OR severe leg and back pain persists.
What does surgery mean to me as a patient?
Using microsurgical techniques, lumbar spine stenosis decompression can now be performed in many cases through a small incision of about 3 cm. The smaller the surgical trauma, at any age considered, but especially in the elderly, the significantly faster the recovery and return to daily activities will be which is especially true for the elderly, where results of minimally invasive surgery are significantly better. Patients only need to spend one night at the hospital after the operation, the next morning a physiotherapist is there to help them to get up and start exercising, after that the patient is released to go home.
We provide world-class neurosurgical treatment for Latvian residents and for international patients. Learn more here if you are an international patient considering having treatment with us.
The venue for surgical interventions is perfectly equipped private hospital in Riga – “Aiwa clinic”.
What are the long-term (4+ years) results of these operations?
In severe lumbar spine stenosis, approximately 80% of patients have good or excellent results at 4 years after surgery. These results are relatively stable and persist in approximately 70% of patients for 10 years after surgery.
Patients who were initially treated conservatively (non-operative) and subsequently underwent surgery did not show worse surgical outcomes.

